 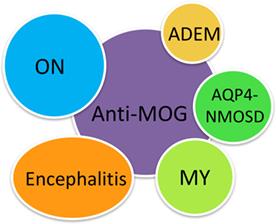
A central cupping could still be recognizedĪnd the majority of the edema appeared to be on the outer side of the optic disc. The optic nerve head appeared to be more swollen ( Figure 3), but the photo was taken several days after presentation. Vision of the left eye progressively decreased to 6/36 after four days. Snellen visual acuity comprised 6/4 and 6/6 for the right and left eye, respectively. The patient was lost to follow-up after four years.Ī 34-year-old male presented with increasing pain of the left eye and headache. Immunosuppression was started six months after presentation by the neurologist (ledertrexate 2×2.5 mg/week-low dose because of lymphopenia and azathioprine was not tolerated). Magnetic resonance imaging scan demonstrated the presence of some aspecific, punctate, hyperintense white matter lesions on T2, but did not show any optic nerve abnormalities. Continued work-up revealed the presence of anti-MOG antibodies. Visual fields normalized as well (MD right eye −1.78 dB/MD left eye −1.77 dB). In the following weeks, Snellen visual acuity restored to 6/6 for the right eye and 6/9 for the left eye (eventually 6/6 after five months). Work-up for infectious causes remained negative and empirical treatment with intravenous corticosteroids was instituted (IV methylprednisolone 1 g/day for 5 days). Again, the edema was most pronounced at the border of the optic disc ( Figure 2). Optic disc edema was noted in the eye fundus, along with some splinter hemorrhages around the left optic disc. Instead, a binocular Esterman was taken with diffuse loss of sensitivity (60/120 not seen periphery relatively spared, but diffuse loss of sensitivity otherwise). Unfortunately, as the patient was seen outside the neuro-ophthalmology clinic, monocular visual fields were not performed. At presentation, visual acuity was counting fingers for the right eye and hand movements for the left eye. For the past week, he had been experiencing a progressive loss of vision, which first started in the left eye and then consecutively also in the right eye. The patient has been followed for four years.Ī 49-year-old male was referred for bilateral optic disc edema (asymmetric, more on the left) after a flu-like episode two weeks before presentation. Additional scanning after 10 days revealed a hyperintense left optic nerve on MRI-FLAIR. Initial MRI scan at presentation did not show any abnormalities, but did not include fluid-attenuated inversion recovery (FLAIR). No other neurological deficits were present. At this point, the patient was still on oral methylprednisolone 48 mg/day and azathioprine 3×50 mg/day was then added for long-term treatment by the neurologist.Ĭlinical neurological examination was unremarkable. Finally, further work-up revealed the presence of anti-MOG antibodies after three weeks. Visual fields also gradually returned to normal (MD right eye −1.13 dB/MD left eye 1.85 dB). In the ensuing days his vision progressively improved to 6/6 in both eyes. The causes of infection could not be demonstrated and intravenous (IV) corticosteroids were started because of the progressive visual loss (IV methylprednisolone 1 g/day for seven days, followed by oral methylprednisolone 64 mg/day and then slowly tapered over the course of three months). Visual fields suggested a right homonymous hemianopia, but progressed to a diffuse and near absolute visual field loss the next day [macular degeneration (MD) right eye −32.47/MD left eye −32.60). Eye fundus demonstrated bilateral optic disc swelling, concentrated around the margins of the optic disc ( Figure 1). 
Snellen visual acuity comprised 6/18 for both eyes. His complaints had started a week before and had progressively deteriorated since then. A 49-year-old male presented to the emergency department in our hospital with complaints of visual loss, headache, and vomiting. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
